Micropatterned Endotracheal Tubes Reduce Secretion-Related Lumen Occlusion
When patients are mechanically ventilated, endotracheal tubes have the potential to disrupt normal airway secretion production and clearance. This ultimately results...... Read More
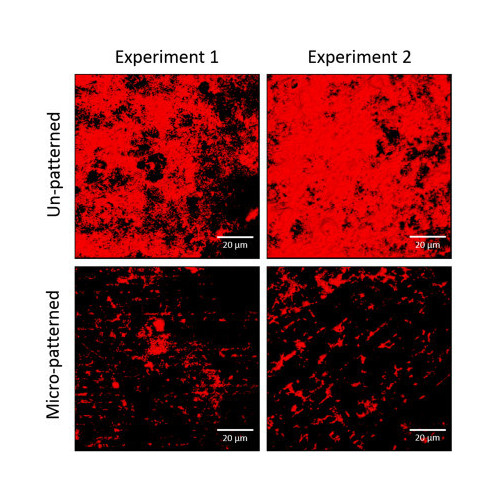
Micro-patterned surfaces reduce bacterial colonization and biofilm formation in vitro: Potential for enhancing endotracheal tube designs (2014)
Background Ventilator-associated pneumonia (VAP) is a leading hospital acquired infection in intensive care units despite improved patient care practices and...... Read More