Sharklet Central Venous Catheter (CVC)
Sharklet uses micropattern alone – no chemicals – to control bacterial biofilm and prevent platelet adhesion and activation.
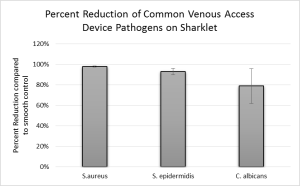
Catheter-related bloodstream infections are associated with 28,000 deaths in the United States every year. The presence of a venous catheter often causes blood clots, beginning with platelet adhesion and activation and ultimately causing deadly clots and embolisms. Treatments with drugs, while effective, can be associated with resistance and contamination.
A Sharklet patterned central venous catheter (CVC) would prevent platelet adhesion and activation while protecting the catheter from infection-causing biofilms. The Sharklet micropattern even inhibits biofilms of deadly fungal pathogens, species which are not affected by antibiotics or typical antimicrobial coatings.
The Research
A smooth surface (left) and a Sharklet patterned surface (right). The Sharklet surface shows 80% less surface coverage of fibrogen, indicating significantly reduced platelet activation.
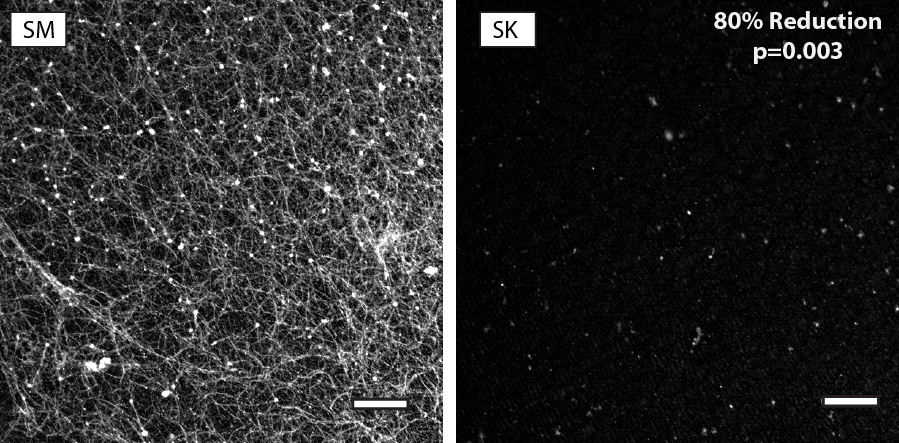

Platelet adhesion on a smooth surface (top) and on a Sharklet micropatterned surface (bottom). The Sharklet patterned surface shows an 82% reduction in platelet coverage.
